Taking Female Health Seriously From Every Angle
Women’s health is not a single specialty — it is an ecosystem. It spans reproductive medicine, hormonal balance, cardiovascular care, mental health, bone density, metabolic function, and preventive screenings that change in priority as a woman moves through different life stages. Yet historically, many of these dimensions have been treated in isolation, leaving women to navigate a fragmented system where no single provider holds the full picture.
The growing demand for “all women’s health & medical services” reflects a shift in how women are approaching their own care — moving away from reactive, symptom-focused visits and toward proactive, integrated relationships with providers who understand the full complexity of female physiology. “All women’s health & medical services” encompasses everything from annual wellness exams and prenatal care to hormone optimization, mental health support, nutritional medicine, and emerging wellness therapies that complement traditional clinical treatment.
Why Comprehensive Care Matters More Than Specialty Silos
The conventional model of healthcare often routes women through a series of disconnected specialists — an OB-GYN for reproductive concerns, a cardiologist for heart health, a psychiatrist for mental health, an endocrinologist for thyroid or hormonal issues. Each provider operates within their lane, and the result is a collection of assessments that rarely speak to each other.
This fragmentation creates gaps. A woman experiencing fatigue, weight gain, mood fluctuations, and disrupted sleep may receive a different partial diagnosis from each specialist she visits, when in reality these symptoms are frequently connected through a single hormonal or metabolic thread. Integrated “all women’s health & medical services” providers are designed to close these gaps by viewing the patient as a whole system rather than a collection of separate complaints.
The practical benefit is faster, more accurate identification of root causes. When a provider can see lab results across hormone panels, metabolic markers, cardiovascular indicators, and mental health assessments simultaneously, patterns emerge that individual specialty evaluations consistently miss. This comprehensive visibility is one of the most compelling reasons to seek out truly integrated women’s health care.
Preventive Screenings and the Lifecycle of Female Health Needs
Preventive care forms the foundation of any serious women’s health strategy, and the specific screenings and priorities shift meaningfully across different life stages. In a woman’s twenties and thirties, the focus typically includes cervical cancer screening, STI testing, reproductive health counseling, and baseline cardiovascular and metabolic assessments.
As women enter their forties, the screening landscape expands to include mammography, bone density baseline measurements, more frequent cholesterol and blood pressure monitoring, and a closer watch on hormonal shifts that signal the approach of perimenopause. The forties are also a decade when thyroid dysfunction becomes more common in women and should be part of routine evaluation.
“All women’s health & medical services” that take a lifecycle approach build screening schedules that anticipate these shifts rather than responding to them after symptoms have already emerged. This forward-looking posture is one of the defining characteristics of high-quality women’s health care and stands in sharp contrast to the reactive model that still dominates much of mainstream medicine.
Hormonal Health as a Central Pillar
Hormones govern an extraordinary range of functions in the female body — mood regulation, sleep architecture, metabolism, bone maintenance, cardiovascular protection, libido, cognitive sharpness, and skin integrity among them. Yet hormonal evaluation is still underutilized in general practice, with many providers treating hormonal complaints as a normal inconvenience rather than a clinically addressable imbalance.
Comprehensive women’s health providers assess a full hormonal panel that includes estrogen, progesterone, testosterone, DHEA, cortisol, thyroid hormones, and insulin markers. The results of these assessments can explain symptoms that have gone unaddressed for years and open pathways to treatment — whether through bioidentical hormone therapy, nutritional interventions, targeted supplementation, or lifestyle modifications that support endocrine function.
Perimenopause and menopause deserve particular clinical attention. The hormonal transition that begins years before menstruation ceases carries symptoms that significantly affect quality of life for many women, yet research consistently shows that these concerns are dismissed or undertreated in clinical settings far more often than comparable male hormonal decline. “All women’s health & medical services” that specialize in this transition offer women a meaningfully better experience and more effective outcomes.
Mental Health, Stress, and the Mind-Body Connection
Women experience depression, anxiety, and stress-related conditions at higher rates than men, and the hormonal dimension of female physiology plays a direct role in this disparity. Fluctuations across the menstrual cycle, the postpartum period, perimenopause, and menopause all create windows of heightened psychological vulnerability that are biologically driven and clinically significant.
Progressive women’s health providers integrate mental health support — whether through in-house therapists, psychiatrists, or coordinated referral networks — rather than treating it as entirely separate from physical health. The connection between chronic stress and immune function, hormonal balance, cardiovascular risk, and inflammatory markers is well established, making psychological wellbeing a clinical concern and not merely a personal one.
Mindfulness-based interventions, cognitive behavioral therapy adapted for hormonal mood patterns, and nutritional psychiatry approaches are all finding their way into the toolkit of forward-thinking “all women’s health & medical services” providers. These integrative approaches recognize that a woman’s mental and emotional state is inseparable from her physical health trajectory.
Emerging Wellness Therapies Expanding the Standard of Care
The definition of women’s health care is broadening to include evidence-informed wellness therapies that complement traditional medicine. IV nutrient therapy, peptide protocols, red light therapy, and various recovery-focused treatments are increasingly offered alongside conventional clinical services in integrative women’s health settings.
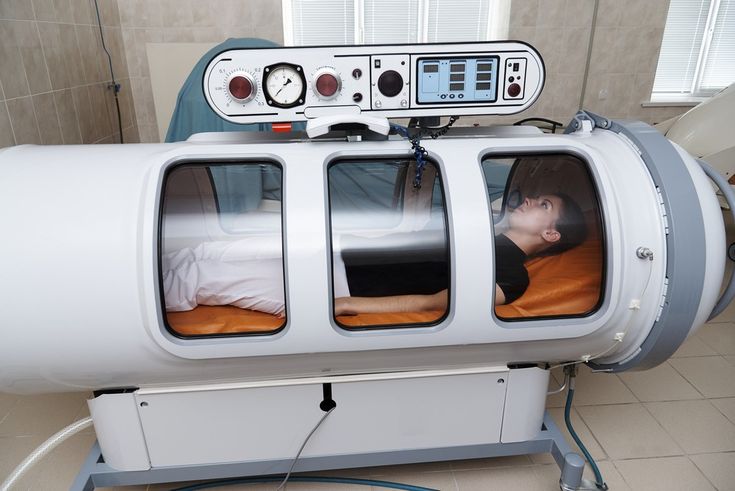
“Oxygen bar treatment” is one such emerging wellness option gaining traction in integrative health spaces, particularly for women managing fatigue, stress, and cognitive fog. Concentrated oxygen sessions are used by some providers to support energy levels, mental clarity, and recovery — appealing to women who are looking for non-pharmaceutical ways to address the daily toll of hormonal fluctuation, sleep disruption, or demanding professional and caregiving schedules.
“Oxygen bar treatment” is typically offered as a complementary therapy rather than a primary medical intervention, and the best providers present it transparently within that context — as a supportive tool rather than a cure. “Oxygen bar treatment” alongside other wellness modalities reflects a broader movement in women’s health toward meeting patients where they are, offering options that support daily functioning and quality of life even when a clinical diagnosis is not the driving concern.
Choosing the Right Provider for Your Full Spectrum of Needs
Finding a practice that genuinely delivers on the promise of “all women’s health & medical services” requires asking direct questions before committing to a provider relationship. Does the practice offer comprehensive hormonal testing, or do they rely on a narrow panel that misses key markers? Are mental health services integrated or referred out entirely? Does the team include a range of specialists — OB-GYN, endocrinologist, nutritionist, behavioral health provider — or is care limited to a single generalist perspective?
Telehealth has expanded access to integrated women’s health care significantly, allowing women in underserved geographic areas to access providers who specialize in hormonal medicine, nutritional health, and preventive care without requiring travel to major metropolitan areas. This democratization of specialized care is one of the most meaningful developments in “all women’s health & medical services” in recent years.
The right practice feels like a partnership. Providers who listen without dismissing, who explain their clinical reasoning, who follow up proactively, and who adapt protocols based on how a patient actually responds are the gold standard. Women deserve that standard — not as a premium offering but as a baseline expectation of what quality healthcare looks and feels like at every stage of life.
A New Standard for How Women Experience Healthcare
The era of accepting fragmented, symptom-reactive care as the norm is ending for a growing number of women who have discovered what genuinely integrated “all women’s health & medical services” can offer. When physical health, hormonal balance, mental wellbeing, preventive strategy, and emerging wellness therapies are coordinated under a unified care philosophy, the outcomes are measurably better and the patient experience is fundamentally different.
Every woman deserves a healthcare relationship that sees her completely — not as a collection of symptoms to be routed to the appropriate specialist, but as a whole person whose health needs are interconnected, evolving, and worthy of serious, sustained clinical attention. “All women’s health & medical services” at its best delivers exactly that — and the providers committed to that standard are reshaping what women believe is possible from their healthcare experience.











Leave a comment